This article underscores the importance of not relying on just one modality to protect us from cancer. Although mammography has been a powerful tool in the fight to detect breast cancer early, it is not the only tool we have and combining a variety of diagnostic and preventative tools is truly the best way to avoid invasive breast cancer.
- Mammography. This test is currently the standard of care for screening for breast cancer. But women must remember that this is an x-ray of the breast. The breast is not an air-filled cavity or a bone so the pictures that are generated are limited. The mammogram is limited by dense breasts, meaning that a small cancerous tumor can be hidden in-between breast tissue. Also, keep in mind that this procedure exposes breast tissue to trauma and radiation, both of which can be cancer causing to this delicate tissue.
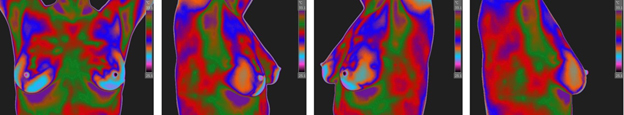
- Thermography-a picture generated by a heat sensing camera. A “hotspot” in the breast can be indicative of angiogenesis, which is the formation of new blood vessels to feed the developing tumor. This is a great way to make healthy lifestyle changes before cancer actually forms or to remove the cancer before it has a chance to spread at all. Breast thermography is not limited by density of breast tissue, making it an excellent test for younger women (20-50 years old). Thermography is underutilized due to its lack of regulation and general acceptance by the medical community. Thermography is intended to be an adjunctive test, not to stand alone from mammography. Thermograms are sometimes done with improper cameras or with improper follow-up. That is why we offer thermography in our office. Our camera is top of the line,
- Self-Breast Exam. Most of the women that I know who have had breast cancer found it themselves. We should never underestimate the power of knowing our own bodies. Women should be encouraged from a young age to know their breasts normal lumps and bumps. When they are older, they will be confident that they will notice any changes in their breasts.
- Prevent breast cancer by breastfeeding and healthy lifestyle choices like exercise and low sugar diets. Studies have shown that the breast is changed by the breastmilk flowing through it. There is actually a component of breastmilk that has an anti-tumor function. The greatest benefit is achieved from breastfeeding when a woman was breastfed as a child and then goes on to breastfeed her offspring. Exercise has been shown to decrease risk for almost all diseases including breast cancer. Sugar causes inflammation and acidity in our bodies; cancer cells love this type of environment and this chemistry change can make a woman’s immune system less able to recognize and eliminate cancer cells (source).
Remember that breast cancer is not limited to women with a family history, all women must be aware of the risk of breast cancer and work toward prevention. Call to day to schedule your Breast Thermography Appointment. Remember Breast Thermography is a non-invasive, radiation-free assessment tool